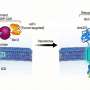
A groundbreaking advancement in cancer treatment has emerged with the development of remote-controlled chimeric antigen-receptor (CAR) T cells that utilize the drug venetoclax to disengage from tumors. This innovative approach aims to enhance the efficacy of CAR-T cells, particularly against solid tumors, which have traditionally posed significant challenges in oncology.
CAR-T cells have already revolutionized the treatment landscape for blood cancers, offering hope to patients who once faced limited options. Nonetheless, their effectiveness against solid tumors, which account for a majority of cancer cases, has been limited. Further complicating their use, these engineered immune cells can inadvertently harm healthy tissues, leading to serious side effects or even life-threatening immune reactions.
Advancing Cancer Treatment with Remote Control
The latest research, conducted by a team of scientists, introduces a method where CAR-T cells can be controlled remotely. By incorporating venetoclax, a drug known for its ability to trigger cancer cell death, researchers aim to minimize collateral damage to healthy cells. This innovative mechanism allows CAR-T cells to disengage from tumor sites when necessary, reducing the risk of adverse effects.
Venetoclax, which has shown promise in treating chronic lymphocytic leukemia, can enhance the therapeutic potential of CAR-T cells. The ability to control these immune cells remotely could significantly improve treatment outcomes for patients battling solid tumors. This advancement reflects a deeper understanding of the immune system’s complexities and the need for precise targeting in cancer therapies.
Potential Impact on Clinical Practice
As this research progresses, it may pave the way for new clinical trials aimed at evaluating the safety and effectiveness of remote-controlled CAR-T cells in diverse cancer types. The implications of such advancements could be profound, transforming the landscape of cancer treatment and offering new hope to patients with solid tumors.
Current treatment protocols often necessitate aggressive approaches that can lead to severe side effects. By enabling CAR-T cells to disengage from non-cancerous cells, this new method seeks to reduce the burden of treatment while maintaining the cells’ ability to combat malignant tumors.
The findings underscore the ongoing evolution of immunotherapy in oncology. As researchers continue to explore the potential of CAR-T cells, the integration of remote control technology may represent a significant leap forward in personalized cancer treatment.
In summary, the development of remote-controlled CAR-T cells using venetoclax highlights the potential for innovative strategies in the fight against cancer. This research not only addresses the limitations associated with traditional CAR-T therapies but also opens up new avenues for improving patient outcomes in solid tumor management. As studies continue, the medical community eagerly anticipates the impact of these advancements on future cancer therapies.