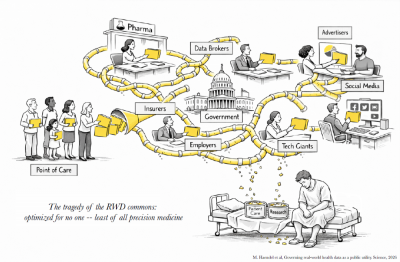
In a groundbreaking paper published by researchers at the University of North Carolina (UNC), a call has been made to govern health data as a public utility. This proposal aims to elevate health data to the status of essential national infrastructure, emphasizing the need for a balance between patient empowerment, privacy, innovation, and the broader public good.
The authors of the paper argue that treating health data as a public utility can significantly enhance the quality of healthcare. By ensuring that data is accessible and used responsibly, the initiative could facilitate better health outcomes and foster innovation in medical research. The researchers emphasize that this approach would not only benefit patients but also empower healthcare providers and researchers to make informed decisions based on comprehensive data.
Balancing Privacy and Public Benefit
One of the central tenets of the proposal is the need to protect patient privacy while maximizing the utility of health data. The researchers highlight that, under the current system, there is often a conflict between individual privacy rights and the collective benefits derived from data sharing. By establishing health data as a public utility, the framework could ensure that data is used ethically and transparently.
The paper outlines several key principles that would guide this governance model. These include prioritizing patient consent, implementing robust security measures, and ensuring that data is used solely for the public good. The authors believe that by adhering to these principles, the initiative can foster trust among patients, encouraging them to share their health information for research and innovation.
Potential for Innovation and Improved Health Outcomes
The proposal also emphasizes the potential for innovation that could arise from treating health data as a public utility. By allowing researchers easier access to comprehensive data sets, the initiative could lead to breakthroughs in various medical fields. The researchers argue that this would not only improve health outcomes but also streamline the development of new treatments and technologies.
Moreover, the authors contend that a public utility model could help address inequalities in healthcare access. By ensuring that all stakeholders, including underserved communities, have access to health data, the initiative could contribute to more equitable health solutions. This approach would align with the growing recognition of social determinants of health and the need for inclusive healthcare strategies.
The UNC researchers are advocating for policymakers to consider this model seriously. They believe that a shift towards viewing health data as a public utility could redefine the landscape of healthcare, making it more collaborative, innovative, and equitable. As discussions around health data governance continue to evolve, this proposal could play a pivotal role in shaping future policies and practices.
In conclusion, the call from UNC researchers to treat health data as a public utility presents a transformative vision for healthcare. By balancing patient empowerment with public good, this initiative could lead to significant improvements in health outcomes, innovation, and equity within the healthcare system.